Medicare / Medicaid is So Confusing
New benefits and plans are emerging every year.
Medicare / Medicaid is So Confusing
New benefits and plans are emerging every year.
USA Health Insurance is complicated

Health insurance options, for people under the age of 65, range from employer sponsored benefits to individual policies through the Affordable Care Act at healthcare.gov.
Government programs for people who qualify for low-income earners and families called Medicaid.
Medicare covers people 65 years and older and special groups of people with disabilities.
Lastly, the active military and veterans receive care through the Veterans Administration.
$899.9B
Medicare income last year
76M+
receive Medicaid sponsored health services
18.4%
people with Medicare benefits nationwide
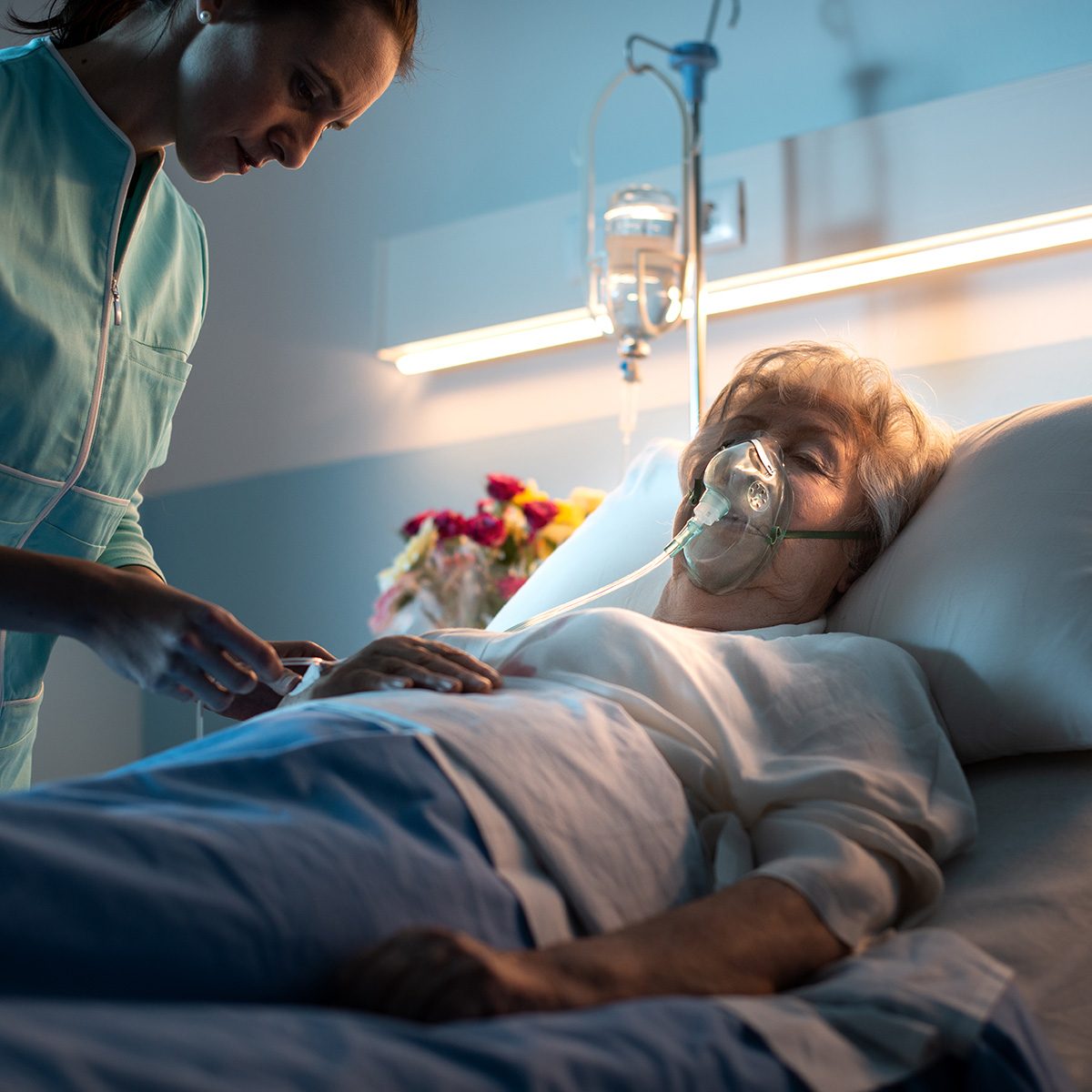
Medicare Part A
Medicare Part A, often referred to as Hospital Insurance, is a fundamental component of the United States’ healthcare program for individuals aged 65 and older. It primarily covers inpatient hospital stays, skilled nursing facility care, hospice services, and some home health care.
Part A benefits include coverage for hospital room charges, nursing services, meals, and necessary medical supplies during an inpatient hospital stay. It also encompasses skilled nursing facility care for rehabilitation following a hospital stay.
Most individuals do not pay a premium for Medicare Part A if they or their spouse have paid sufficient Medicare taxes while employed. However, there are cost-sharing elements such as deductibles and coinsurance.
It’s important for consumers to understand that while Part A offers crucial coverage for inpatient services, it doesn’t cover all healthcare expenses. Additional Medicare coverage, such as Part B (Medical Insurance) for outpatient services, and supplemental plans, may be advisable to ensure comprehensive healthcare coverage. It’s recommended that individuals approaching Medicare eligibility thoroughly review their healthcare needs and available options to make informed decisions about their coverage.

Medicare Part B
Medicare Part B, known as Medical Insurance, is a vital component of the United States’ healthcare program for individuals aged 65 and older. It covers a range of outpatient services, preventive care, and medically necessary services that are not confined to a hospital setting.
Part B benefits include doctor visits, outpatient care, preventive services such as vaccinations and screenings, ambulance services, and durable medical equipment like wheelchairs or walkers. It also covers certain outpatient prescription drugs, particularly those administered in a clinical setting.
Unlike Part A, Medicare Part B requires a monthly premium payment, and the amount is based on income. Additionally, beneficiaries are responsible for an annual deductible and a percentage of the cost-sharing through coinsurance or copayments.
Enrolling in Part B is optional, but it’s advisable for most individuals to consider this coverage to ensure comprehensive healthcare. It’s crucial for consumers to carefully review their healthcare needs, understand the associated costs, and enroll during their Initial Enrollment Period to avoid potential late enrollment penalties. Supplemental plans may also be explored to enhance coverage and reduce out-of-pocket expenses.

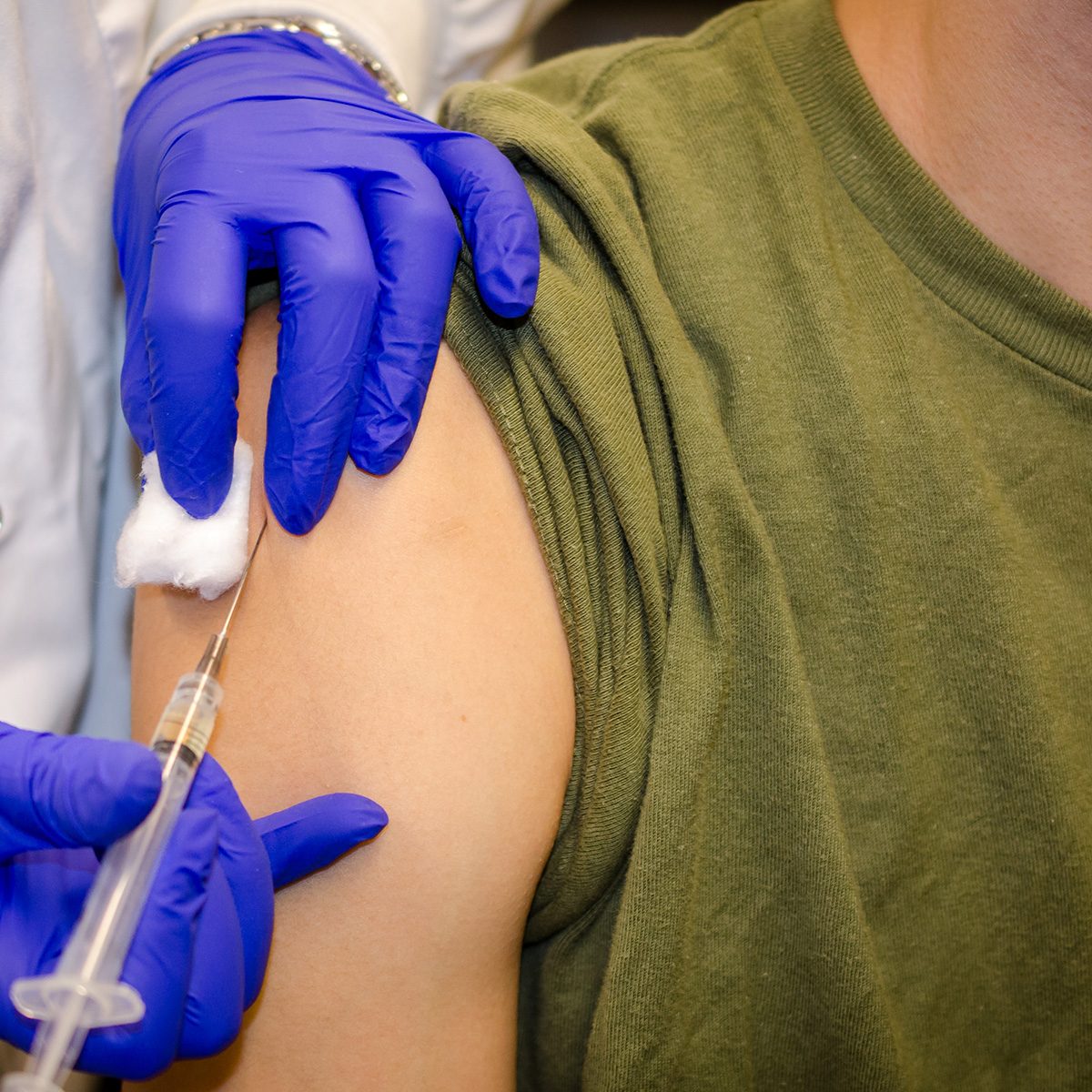
Medicare Part C also known as Medicare Advantage
Medicare Part C, also known as Medicare Advantage, offers an alternative approach to traditional Medicare coverage. Administered by private insurance companies approved by Medicare, Part C combines the benefits of Part A (Hospital Insurance) and Part B (Medical Insurance) into a single plan. In addition, many Medicare Advantage plans often include prescription drug coverage (Part D) and may offer additional perks such as dental, vision, and fitness benefits.
Consumers opting for Medicare Advantage should understand that they still retain their Medicare rights and protections, including the right to appeal decisions. While Medicare Advantage plans may have lower premiums, they often involve cost-sharing through copayments, deductibles, and coinsurance.
Enrolling in a Medicare Advantage plan requires being eligible for both Part A and Part B, residing in the plan’s service area, and not having end-stage renal disease (with some exceptions). Individuals considering Medicare Advantage should carefully compare plan options based on their healthcare needs, preferred providers, and budget constraints. It’s important to review the plan’s coverage network and potential out-of-pocket costs before making a decision.

Medicare Part D
Medicare Part D is the prescription drug coverage component of the United States’ Medicare program. Offered through private insurance companies approved by Medicare, Part D helps beneficiaries afford the costs of prescription medications. This coverage is available as a standalone Prescription Drug Plan (PDP) for those with Original Medicare (Part A and Part B) or as part of a Medicare Advantage plan (Part C).
Part D plans vary in terms of covered medications, costs, and pharmacies in their network. Beneficiaries pay a monthly premium for Part D coverage, and out-of-pocket costs include annual deductibles, copayments, and coinsurance. There is also a coverage gap, often referred to as the “donut hole,” where beneficiaries pay a higher percentage of the drug costs until catastrophic coverage kicks in.
Enrollment in a Part D plan is voluntary but highly recommended for individuals with Medicare to ensure access to affordable prescription medications. It’s essential for consumers to carefully review plan options each year during the Annual Enrollment Period to ensure their chosen plan aligns with their medication needs and budget constraints.


Special Needs Plan for Dual Enrolled Medicare and Medicaid
A Dual Eligible Special Needs Plan (D-SNP) is a specialized type of Medicare Advantage plan designed for individuals who qualify for both Medicare and Medicaid. Often referred to as dual eligibles, these individuals face unique healthcare needs, as they are typically seniors or disabled individuals with low incomes. D-SNPs are tailor-made to address the specific challenges and provide comprehensive coverage for this population.
Key features of Dual Eligible Special Needs Plans include combining the benefits of both Medicare (Part A and Part B) and Medicaid, offering additional services not covered by Original Medicare. These plans commonly include prescription drug coverage (Part D) and may also provide extras such as dental, vision, and hearing benefits.
Enrollment in a D-SNP is typically available to individuals who meet both Medicare and Medicaid eligibility criteria. D-SNPs aim to streamline healthcare delivery for dual eligibles, enhancing coordination between Medicare and Medicaid services, and often reducing out-of-pocket costs.
Consumers considering a D-SNP should carefully review plan options to ensure they meet their specific healthcare needs, including prescription medications and any additional services offered. The goal of these plans is to improve healthcare outcomes for individuals with dual eligibility, simplifying access to necessary medical services and support.

Medicaid
Medicaid is a joint federal and state program designed to provide health coverage for low-income individuals and families. Administered by individual states within federal guidelines, Medicaid offers a range of comprehensive health services at little to no cost for eligible beneficiaries. While federal standards outline essential coverage requirements, states have flexibility in shaping their specific Medicaid programs.
Medicaid covers a broad spectrum of healthcare services, including hospital and doctor visits, preventive care, prescription drugs, maternity care, mental health services, and long-term care. Eligibility is determined based on income, household size, and other factors, with certain vulnerable populations like pregnant women, children, and individuals with disabilities automatically qualifying.
Expansion of Medicaid under the Affordable Care Act (ACA) extended coverage to more low-income adults in participating states. Enrollment is open year-round, and individuals can apply directly through their state’s Medicaid program.
It’s crucial for consumers to check their state’s Medicaid eligibility criteria and application process. Medicaid plays a vital role in ensuring access to healthcare for those who may not afford private insurance, providing a safety net for millions of Americans with limited financial resources.

Notes from the Author

Program of All-Inclusive Care for the Elderly (PACE)
Some States have PACE, Program of All-Inclusive Care for the Elderly, a Medicare program that provides care and services to people who otherwise would need care in a nursing home. PACE covers medical, social service, and long-term care costs for frail people. It may pay for some or all of the long-term care needs of a person with Alzheimer’s disease. PACE permits most people who qualify to continue living at home instead of moving to a long-term care facility. You will need to find out if the person who needs care qualifies for PACE. There may be a monthly charge. PACE is available only in certain States and locations within those States.
State Health Insurance Assistance Program (SHIP)
SHIP, the State Health Insurance Assistance Program is a national program offered in each State that provides counseling and assistance to people and their families on Medicare, Medicaid, and Medicare supplemental insurance (Medigap) matters.
Department of Veterans Affairs
The U.S. Department of Veterans Affairs (VA) may provide long-term care or at-home care for some veterans. If your family member or relative is eligible for veterans’ benefits, check with the VA or get in touch with the VA medical center nearest you. There could be a waiting list for VA nursing homes.
Social Security Disability Income (SSDI)
This type of Social Security is for people younger than age 65 who are disabled according to the Social Security Administration’s definition.
For a person to qualify for Social Security Disability Income, he or she must be able to show that:
- The person is unable to work
- The condition will last at least a year
- The condition is expected to result in death
Monica Stynchula – CEO / REUNIONCare, Inc.













